
Intracranial (bleeding) Hemorrhage Treatment in Thane
Intracranial (bleeding) hemorrhage is a medical condition of utmost urgency requiring immediate expert handling. High-tech neuro-surgical methods that incorporate precise imaging and various for certain bleed areas make up the mainstay of the treatment of these intricate cases. The certain way of treating the bleed depends on its site, volume, and type.
Dr. Naren Nayak, a prominent neurosurgeon in Thane known for his work in functional neurosurgery, states, “The outcome of intracranial hemorrhage to a large extent relies on prompt surgical intervention, we are still aspiring to combine with the latest surgical techniques to give the best recovery.”
What makes intracranial hemorrhage such a critical condition? Let’s delve into the fundamental aspects of this neurological emergency.
Overview of Intracranial Hemorrhage
Intracranial hemorrhage is a grave emergency marked by bleeding within the skull, which exerts pressure on brain structures and disrupts neurological function. It accounts for about 8-13% of all strokes and is associated with higher morbidity and mortality than other stroke types.
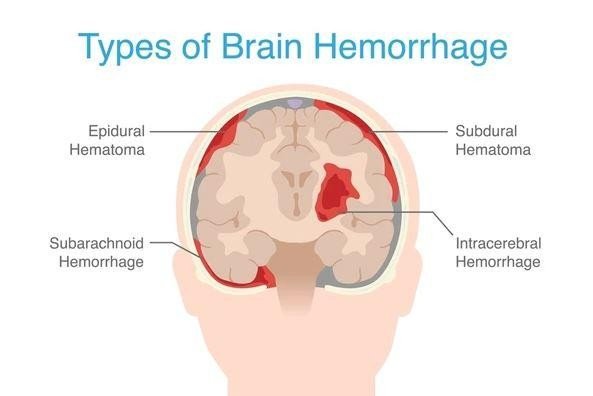
Types of Intracranial Hemorrhage
We classify intracranial hemorrhage by bleed location.
Intracerebral hemorrhage involves bleeding within the brain tissue itself, sometimes extending to the ventricles.
Subarachnoid hemorrhage occurs in the space between the brain and its membrane.
Read More..
Subdural hematoma forms between the brain’s outer covering and the brain
Epidural hematoma develops between the skull and the outer membrane.
Each type presents its own challenges and demands a tailored treatment plan.
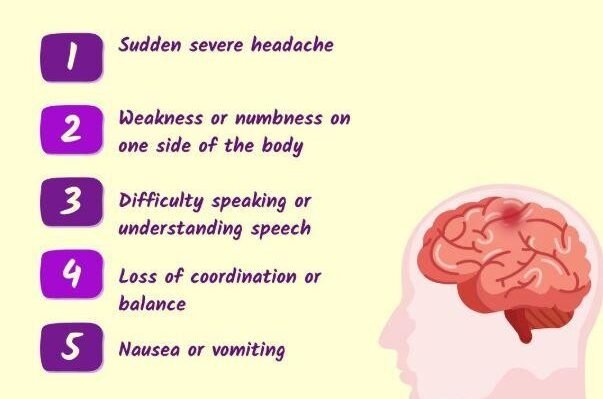
Symptoms and Warning Signs
The intense headache usually foreshadows the other symptoms and is sometimes characterized as the most painful headache one could possibly have. Apart from the headache, a patient can also show rapid onset of confusion, talking found hardest or speaking unclear, or having loss of sensation on one side of the body. Patients with headache may also complain of visual disturbances such as blurred or double vision.
Read More..
In cases where the bleeding is massive, the patient might be unconscious or have a very mild form of altered consciousness. On the other hand, if the bleeding is large, the patient might have seizures. Nausea and vomiting are frequently symptoms that indicate increased intracranial pressure, and hemiparesis might develop as a result of the blood compressing certain areas of the brain.
Glasgow Coma Scale is the primary method used to evaluate the state of consciousness, where scores that fall below 8 mean life-threatening condition.

Common Causes and Risk Factors
Chronic hypertension is the primary cause of spontaneous intracerebral hemorrhage. Persistent high blood pressure weakens vessel walls, predisposing them to rupture. This risk is heightened in patients with poor blood pressure control.
Anticoagulant medications (such as aspirin and clopidogrel) increase bleeding risk, especially alongside hypertension.
Read More..
Older adults are at higher risk due to vascular fragility. Traumatic head injuries, vascular malformations like aneurysms or AVMs, and blood clotting disorders can all contribute. Substance misuse, particularly stimulants, is also a notable factor.
How do medical professionals in Thane identify this serious condition? Let’s explore the diagnostic methods used to detect intracranial bleeding.
Diagnosis of Intracranial Hemorrhage in Thane
Accurate diagnosis relies on advanced imaging and detailed clinical evaluation to determine bleed extent and guide management. We integrate modern diagnostic tools with comprehensive neurological assessments for each patient.
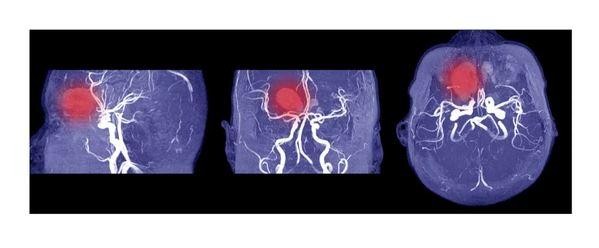
Diagnostic Imaging Techniques
Computed Tomography (CT) scans
are the first-line diagnostic tool for intracranial hemorrhage. Their speed and sensitivity to acute bleeding make them indispensable in emergencies.
CT imaging delineates the hemorrhage’s location, size, and type, and reveals mass effect or midline shift. This allows us to distinguish between subdural, epidural, intracerebral, and subarachnoid bleeds.
Magnetic Resonance Imaging (MRI)
offers greater detail for brain tissue assessment and can pick up subtle or chronic bleeds. MRI is reserved for cases where additional information is needed beyond CT findings.
CT angiography
is used to identify bleeding sources, particularly when vascular abnormalities are suspected. It involves contrast dye to visualize vessels and pinpoint ruptures.
We use the Glasgow Coma Scale (GCS) to gauge consciousness and neurological function, scoring eye, verbal, and motor responses from 3 to 15.
A GCS below 8 signals severe impairment and the need for urgent action. Ongoing GCS monitoring helps track changes in status.
Physical examination includes:
Pupil reactivity and size
Motor strength bilaterally
Sensory function
Reflexes to assess brainstem
Speech and language
Evaluating Severity and Treatment Approach
We calculate hematoma volume from imaging; clots over 30 ml often require surgical evacuation.
Midline shift greater than 5 mm is a significant indicator for surgical decompression.
Additional considerations include:
Patient age and comorbidities
Blood pressure and medication use
Time since symptom onset
Rate of neurological decline
Which treatment approaches prove most effective for managing brain hemorrhages? Let’s discuss the comprehensive options available to patients.
Intracranial Hemorrhage Treatment Options
Non-Surgical Management
Blood pressure control is the foundation of conservative treatment. We aim to keep systolic pressure below 140 mmHg to limit hematoma expansion while maintaining cerebral perfusion.
For patients on anticoagulants, reversal is initiated immediately—using vitamin K, prothrombin complex concentrate, or specific antidotes as appropriate.
Close monitoring in intensive care, with frequent neurological checks and repeat imaging, is essential. Smaller hematomas without mass effect often resolve with medical therapy.
Supportive care may include:
- Intracranial pressure monitoring
- Seizure prophylaxis
- Temperature and glucose management
- Prevention of complications
Surgical Interventions
Surgery is indicated when hematoma volume exceeds 30 ml, midline shift is over 5 mm, or GCS drops below 8. These criteria reflect critical pressure and risk to life.
Craniotomy is the standard surgical approach, involving temporary removal of part of the skull to evacuate blood. The bone flap is preserved for later replacement, usually within three months.
Minimally invasive options, such as stereotactic aspiration or endoscopic evacuation, are reserved for certain cases based on bleed location and consistency.
Decompressive craniectomy is considered if significant swelling persists after evacuation, to prevent herniation.
Postoperative Care and Monitoring
Following surgery, patients require intensive care with ventilatory support and continuous neurological observation. Regular imaging is used to detect rebleeding or hydrocephalus.
Typical postoperative complications include:
- Ventilator-associated pneumonia
- Surgical site infection
- Pressure ulcers
- Postoperative seizures
Early physiotherapy is started to address hemiparesis and reduce contracture risk. Comprehensive rehabilitation supports motor recovery, especially in those with good preoperative function.
Long-term care involves skull bone replacement and strict blood pressure management to reduce the risk of recurrence.
For patients in Thane, Dr. Naren Nayak’s combination of advanced training, clinical experience, and ongoing research ensures high standards in intracranial hemorrhage management.
How does Dr. Nayak’s specialized training benefit patients with intracranial bleeding? Let’s discover his unique approach to neurosurgical intervention.
Role of Neurosurgeon Dr. Naren Nayak in Thane
Emergency neurosurgical interventions for hemorrhagic strokes
Our Approach & Procedure
We start with prompt diagnostic imaging to assess the hemorrhage’s size, location, and severity. Key parameters, such as hematoma volume, midline shift, and the patient’s Glasgow Coma Scale score, guide our initial evaluation.
Our surgical intervention involves:
- Craniotomy– Removing a section of skull to access the affected brain region
- Hematoma evacuation– Clearing accumulated blood to alleviate pressure
- Skull preservation– Maintaining the bone flap in sterile storage for later replacement, usually within three months
Throughout the process, we focus on blood pressure regulation to prevent rebleeding. Monitoring continues in intensive care, tracking intracranial pressure and neurological status around the clock.
Post-operative care includes:
- Ventilator support if indicated
- Prevention of infections and bedsores
- Early mobilisation protocols
- Seizure prophylaxis when required
Aggressive physiotherapy is introduced early to address motor deficits. Many patients face weakness or paralysis on one side, and our rehabilitation strategies are designed to optimise recovery of function.
Our multidisciplinary team coordinates neurosurgical, critical care, and rehabilitation services. We maintain regular communication with families, providing updates on prognosis based on hematoma characteristics, comorbidities, and response to intervention.
What does the healing journey look like after neurosurgical intervention? Let’s explore the rehabilitation process and expected outcomes.
Recovery and Rehabilitation After Hemorrhage
Rehabilitation after intracerebral hemorrhage requires structured support across multiple domains, from restoring physical function to monitoring for delayed complications. About half of survivors experience significant disability, so rehabilitation remains central to reducing impairment and restoring independence.
Physical Rehabilitation Programmes
Physical rehabilitation begins as soon as it’s safe, often within days of stabilisation. Early mobilisation helps lower the risk of pneumonia, deep vein thrombosis, and muscle atrophy, while leveraging neuroplasticity in the initial three months post-hemorrhage.
Core rehabilitation components include:
- Physiotherapy for mobility, balance, and strength
- Occupational therapy to promote independence in daily activities
- Speech and language therapy for communication and swallowing
- Cognitive rehabilitation to address attention, memory, and executive function
Therapy intensity and duration depend on hemorrhage location, size, and pre-existing function. Motor improvement often continues for up to six months, with upper limb recovery typically trailing behind lower limb gains. Sensory deficits and truncal control may plateau by three months.
Long-Term Health Monitoring
Long-term recovery requires regular follow-up to monitor neurological status, manage risk factors, and identify complications early. Blood pressure control is critical, as hypertension remains the leading cause of recurrent hemorrhage.
We aim for blood pressure below 130/80 mmHg, schedule neuroimaging at intervals to monitor hematoma resolution, and screen for depression and cognitive dysfunction—issues affecting a significant proportion of survivors.
Medication adherence and anticoagulation strategies are reviewed as needed, balancing stroke prevention with bleeding risk. Lifestyle changes, such as dietary adjustments, exercise, and smoking cessation, are integral to long-term care.
Managing Postoperative Complications
We monitor for both early and delayed complications following surgery. Immediate risks include wound infection, cerebrospinal fluid leakage, and seizures, which occur in roughly 10-15% of cases.
Common complications requiring management:
| Complication | Timeframe | Management Approach |
| Hydrocephalus | Days to weeks | Ventriculoperitoneal shunting if persistent |
| Seizures | Days to months | Antiepileptic medications |
| Spasticity | Weeks to months | Botulinum toxin, baclofen, physiotherapy |
| Cognitive deficits | Ongoing | Cognitive remediation therapy |
Spasticity is managed with oral medications, botulinum toxin injections, and targeted physiotherapy. Cognitive dysfunction needs specialised rehabilitation focusing on memory, attention, and executive functions. Depression screening is routine, as emotional health strongly influences overall recovery.
What common concerns do patients have about intracranial hemorrhage treatment? Let’s discover answers to the most frequently asked questions.
Frequently Asked Questions
What are the latest advancements in the treatment of intracranial hemorrhage?
Minimally invasive techniques like stereotactic aspiration and endoscopic evacuation, combined with intraoperative imaging, robotics, and advanced hemostatic agents, have reduced surgical trauma while improving precision, safety, and recovery times.
Can you detail the surgical and non-surgical options available for intracranial hemorrhage?
Surgical options include craniotomy, burr hole drainage, endoscopic evacuation, and decompressive craniectomy. Non-surgical management is reserved for smaller, stable hematomas and focuses on medical therapy and monitoring.
What factors influence the choice of treatment for a patient with an intracranial hemorrhage?
Key factors include hematoma volume, Glasgow Coma Scale score, mass effect, patient age, comorbidities, and blood pressure control. These guide whether surgical or conservative management is appropriate.
What is the recovery process like after undergoing treatment for intracranial hemorrhage?
The first period of recovery in ICU consists of checking one’s condition closely and often giving one ventilator support during the process, later physiotherapy to tackle the most common deficits like hemiparesis is given when the patient is stable. Skull replacement takes place about three months after surgery with long-term recovery differing a lot depending on the hematoma characteristics and personal factors.
What is the recovery process like after undergoing treatment for intracranial hemorrhage?
The first period of recovery in ICU consists of checking one’s condition closely and often giving one ventilator support during the process, later physiotherapy to tackle the most common deficits like hemiparesis is given when the patient is stable. Skull replacement takes place about three months after surgery with long-term recovery differing a lot depending on the hematoma characteristics and personal factors.
How do you assess the severity of an intracranial hemorrhage before deciding on a treatment plan?
CT scanning rapidly visualizes hemorrhage size, location, and volume (>30ml prompting intervention), while Glasgow Coma Scale scoring and midline shift measurement (>5mm indicating urgency) guide surgical decisions. Blood pressure monitoring and coagulation tests identify underlying causes and inform safe treatment planning.
What are the potential risks and complications associated with different intracranial hemorrhage treatments?
Rebleeding from uncontrolled hypertension, ventilator-associated pneumonia, surgical site infections, and seizures from brain injury are major post-operative risks requiring vigilant management. Prolonged immobility also increases the risk of pressure sores, necessitating preventive care and positioning protocols.
Disclaimer: The information shared in this content is for educational purposes only and not for promotional use.
